Imaging beliefs
In today’s society full of technological advancements, medical imaging has become very common and typically readily accessible for the general population. In many cases, medical imaging is great because it assists health care providers in finding or diagnosing pathologies and other conditions. However, in some cases (especially with musculoskeletal injuries/pain) medical imaging has created great misconceptions amongst the public and patients that has led to misguided medical choices that resulted in disappointing or underwhelming outcomes.
Medical imaging
So what is “medical imaging”?
Medical imaging is the process or technique of creating a visual representation of the interior of the body for clinical analysis and/or medical intervention.
Types of Medical Imaging
There are many types of imaging present in modern healthcare, but the most common ones utilized with orthopedic or musculoskeletal conditions are MRIs, X-Ray, and CT scans.
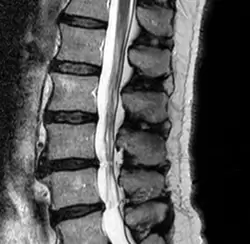
MRI (Magnetic Resonance Imaging): Utilization of strong magnetic fields to create anatomical images. Most commonly used to view soft tissue structures which includes, but is not limited to: ligaments, tendons, muscle, discs, cartilage, neural tissue, etc.
X-ray: Rays of electromagnetic energy/radiation projected through the body to create an image. Most commonly utilized to view images of boney structures, disc/joint space (insight on cartilage status), pneumonia, and even tumors in some cases. X-rays DO NOT show discs, ligaments, muscles, tendon, or other soft tissue structures.
CT (Computed Tomography) Scan: Computer process that compiles x-ray images to create cross sectional images. Typically used for internal head injuries, internal dysfunctions, complex fractures, and other medical conditions.
Evidence of Medical Imaging
Countless times many of us have heard of disappointing results from surgeries, injections, or other treatments for musculoskeletal/orthopedic related conditions, but why? If the treatment performed is fixing what is seen on medical imaging, why is the pain still present?
Many times reason is because what was treated or “fixed” may of not been what had been causing the pain in the first place. A plethora of recent scientific articles and studies have shown that with musculoskeletal pain there is often limited correlation between the results of medical imaging with the origin and severity of pain.
In a group of 49 individuals with all asymptomatic knee osteoarthritis 76% of them had a meniscus tear.
Knee Osteoarthritis Study (CLICK FOR LINK)
“Signs of degeneration are present in very high percentages of healthy people with no problem at all. Many imaging-based degenerative features are likely part of normal aging and unassociated with pain”
In a group of people without shoulder pain (ages ranging from 19 to >60 years old), 34% of them had a partial or complete rotator cuff tear. 54% when only looking at 60 years old or older.
Shoulder Study (CLICK FOR LINK).
Effect on Practice
So how does a physical therapist or other medical professionals treat without knowing what the imaging says? Through a thorough history and physical exam a medical professional is able to determine appropriate treatments and interventions.
- History: Clinicians are well educated on how to take a detailed history and ask guided questions on the mechanism of injury, history of condition/pain, and patterns of symptoms in order to assist them in determining an appropriate diagnosis in conjunction of physical exam findings.
- Physical Exam: Through palpation, range of motion, strength assessment, and special tests*, clinicians are able to use this information to assist them in making a diagnosis.
*Special tests performed in the physical exam portion of evaluations have very similar reliability and validity in diagnosing orthopedic conditions when compared to medical imaging.
Most importantly a physical therapist will treat YOU. Just because imaging shows a pathology does not mean this is why you are suffering. YOU are NOT your MRI.
To speak to a physical therapist, CLICK HERE!
When is Medical Imaging Appropriate?
Medical imaging is a great diagnostic tool, but in some cases (typically musculoskeletal) it is over utilized or too heavily relied on to guide or make medical treatments and decisions.
So this may be leaving you with the question of when is imaging appropriate?
Typically, imaging is most appropriate or warranted in times of:
- Trauma
- Life-threatening conditions/symptoms
- When a condition/pain does not respond to typical treatments or interventions
(Please always consult your physician if imaging is appropriate for your condition and/or injury especially in the circumstances stated above)
Is this why insurances often refuse to pay for imaging?
Yes! In light of all the scientific studies, insurances are hesitant to pay for imaging due to excessive medical costs that will most likely not change the treatment course for that particular condition.